Reflections on COVID-19: The Impact on MS-III’s
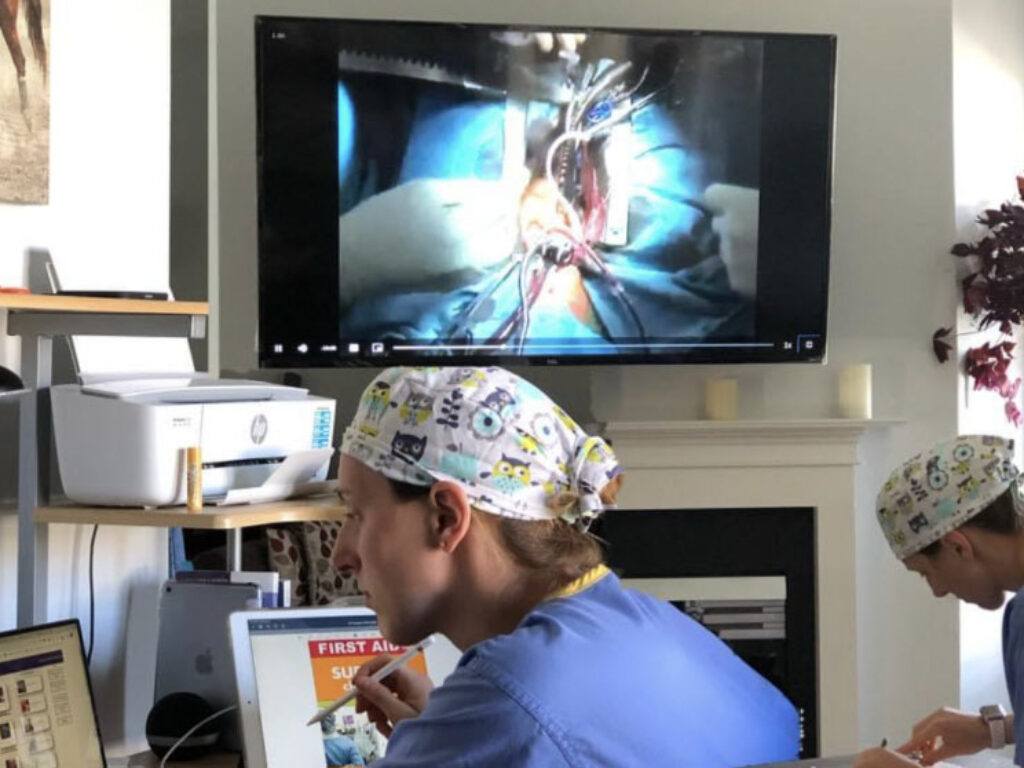
When Shelter-In-Place was ordered in March, and Campbell University moved all instruction to online, Meredith Culbertson was an MS-III enjoying rotations at Cape Fear Valley Health – providing care and learning in the hands-on, dynamic atmosphere that is the rich reward after two years in lecture and lab. Meredith shares the challenges COVID-19 brought to the second half of her third year and the anxieties she and her classmates have as they prepare to apply for residency
What is the difference between MS-I/II years and MS-III/IV years of medical school?
MS-I/II years are primarily lecture and lab instruction. When we apply to med school and throughout our first two years, all many of us do is dream about getting into the hospital – finally getting to clinical rotations. The reason we stress and study ridiculous hours those first two years (and then those excruciating months at the end of 2nd year when we are preparing for boards) is to make it to clinical rotations – its like a mini graduation! It’s a huge victory, and you feel proud of what we are doing.
For me, I believe the amount we learn in clinical years is enormously different and more helpful. Now when I see a question, I can actually picture that patient because I’ve had that patient. I feel very confident about how to treat that patient in real life or in a board style question because now I have had that experience. COVID-19 ripped that away from us and put us back into first and second year.
As MS-IV’s, typically we would spend months on away rotations in preparation for applying for residency in the spring. Medical schools nationally are struggling to figure out what the process is going to be and most of us are very stressed about our schedules and requirements. We just don’t know if we are even going to be able to do away rotations. I am pursuing Emergency Medicine, and we need a specialized Standardized Letter of Evaluation (SLOE) – without it you struggle to get into certain programs. Emergency Medicine Resident Association (EMRA) is working with all the program directors to be more lenient like other residencies (family medicine, pediatrics, etc.) to accept letters from non-residency emergency departments to help us through the application process. They are limiting everyone to one ED rotation to make sure everyone across United States has at least one rotation through an emergency department with a residency before the Match. So, for my class when it comes to The Match, there are just a lot of unknowns and that heightens the stress and frustration.
How did COVID-19 change your MS-III year?
I feel like COVID-19 has stolen our education from us because what we’ve been doing the past few months is not real rotations. It was very frustrating for us because we felt like we went backwards – back to the classroom and lectures in front of a computer versus being in the hospital learning from life experiences. Many of us struggle to learn from books and lecture, but excel in clinical. For me personally, I really excelled for 8-9 months on rotations, and I struggled to not loose motivation and inspiration when that was suddenly taken away.

So, a lot of us were very frustrated and were complaining – especially in the beginning when everything was constantly changing. But, we had to remind ourselves that we are the lucky ones because we still have opportunities to help people in other ways – some people signed up to babysit, to deliver groceries, we did a pediatric supply drive – and we will soon have jobs that will make a huge difference.
How would you say you have been affected personally?
I am a very sociable person and being kinda isolated doing everything remotely has been hard. It definitely messes with your psyche sometimes. I knew going into this career there’s a chance that we might get sick and even really ill – I feel like I know that better than most because I’m immunocompromised. This is not your normal sickness. We all need to be careful and abide by the guidelines, but sometimes it’s really hard and frustrating when all you want to do is to get back into the hospital and help.
Also, my sister is a physician in Colorado. She has MS and had COVID-19 for a month. She’s had to live separately from her husband since that time because he is an anesthesiologist and early on had to provide his own PPE. It was very stressful for them – living a part and making sure she didn’t get reinfected. So, as students, we have to remember people like them and consider ourselves lucky and not complain because it could be so much worse.

What do you think we can learn from COVID-19?
I think it’s been a learning experience for everyone on how to grow and learn with the new normal. We can’t be mad with what has happened. There are still so many opportunities for us to help in other capacities and that’s all we can do right now. Sit down and get through the grunt work knowing that at some point we will get back what we had. We just have to look at the here and now and hope the best for the future knowing we’re all in this together.
Your MS-III year officially ended on June 30th. What was that last month like?
I just tried to focus on studying for boards – fingers crossed my boards don’t get cancelled. I will have to travel to Louisville, KY to take them. I continued taking my dog to the park and survived another month on alternative schedule.
I was supposed to be on surgery my last month as an MS-III. This is what I shared on Facebook the last day of rotations:
‘Today is bittersweet. We are doing the right thing by sheltering in place due to COVID-19, but today was supposed to be the start of my last rotation in the hospital as. 3rd year medical student. Instead of doing surgeries in the hospital, I am making the most of it by hunkering down in the books, practicing my skills, and watching surgeries. We must stay positive and find new ways to challenged ourselves and continue our education to advance our medical careers. So, this month, I will not complain, but make the best of it…virtual surgery.’
Now, I am back in the hospital and it’s been great, but also very weird. It’s like riding a bike. You learned how, but you’ve lost some of the skill, so you’re stumbling through how to do it again – and now there are lots of new guidelines especially in the emergency department.
N 95 masks do give you bruises, but I don’t care that I get bruises or feel tired because this is what I want to do. I love learning something new every day and working hard. I get to be in a place that I feel I belong, and I fit in with a great group of people that are just like me. There are amazing people here at Cape Fear Valley Health who go above beyond.
I’m still very nervous about this residency application season and how it will unfold with all four of my audition rotations being canceled. I have a lower board score, so I wanted to make sure I can show them in person how I excel in hopes they will look past my board score. Again, it’s just very much an unknown, but we have some really good attendings who are understanding and working with us, so I’m hopeful.


